Babies and eczema
Eczema is not unusual in babies, but there is a lot of conflicting advice out there. Julie Van Onselen answers 10 common questions about eczema in little ones. This article was published in Exchange 181, September 2021.
Eczema affects around 20% of children in the UK. It usually starts during the first six months. If your baby is one of them, you may already have experience of eczema in your family – or it may be a brand new condition to get to grips with. These are the most common questions that we tend to hear from families whose babies have eczema.
1. What caused my baby’s eczema?
There is no single cause of atopic eczema. Eczema is a complex condition – it is genetic but also involves an overactive immune response to environmental factors, which cause eczema flares. Because the atopic gene is hereditary, it runs in families, and is responsible for three conditions: eczema, asthma and hay fever.
Fifty per cent of people with eczema have an additional genetic element – a difference in a skin protein called filaggrin – which leads to further problems in the skin barrier. All atopic conditions can be linked to allergies in some people, but there are also many universal irritants, such as soap and heat.
2. Did my baby develop eczema because I couldn’t breastfeed?
As eczema is caused by genetic factors, bottle-feeding a baby definitely cannot cause eczema. In fact, current research is divided, with some studies showing positive effects of breastfeeding and others showing no significant effects at all.
Neither is there enough evidence to advise pregnant or breastfeeding women to avoid specific foods to protect unborn children from atopic eczema or any other atopic condition.
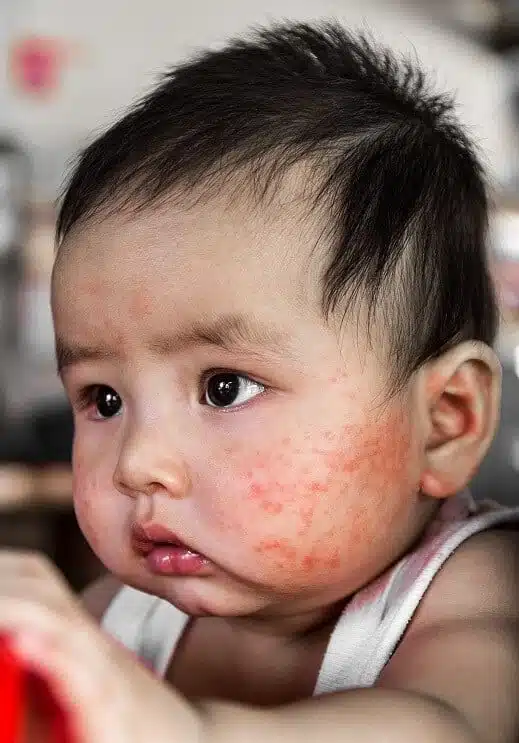
3. What does eczema look like?
In babies with paler skin, when eczema is flaring the skin is red and itchy. In babies with darker skin, the irritated, itchy areas may be red but are more likely to show as darker (hyperpigmented) patches. They may also appear paler around the front or back of knees or elbows.
When an area of darker skin is treated for eczema, it may become lighter and may take several months to return to the baby’s normal skin tone.
4. Will my baby grow out of eczema?
Sadly, it is impossible to predict whether your baby will have eczema for life or for just a short time. So far, there is no cure for eczema. Eczema is a chronic condition with periods of flare and periods of remission, and most people with a history of eczema still have problems with dry and itchy skin. If your child has a difference in their filaggrin gene, they will not grow out of it. Even if your baby appears to ‘grow out of’ their eczema, it may return during the teenage years or in adulthood.
5. Is milk or food allergy a problem and should I make any changes to my baby’s diet?
Dietary allergy can occur in any child – usually between three months and two years of age. Babies with eczema have a slightly higher risk of allergy, but lots of babies with eczema have no milk or other food allergy.
A baby with an immediate allergic reaction may have a sudden flare of eczema, become very itchy or start to wheeze, while a baby with a delayed reaction is more likely to have colic, reflux, vomiting and reluctance to feed.
If you think your baby has a food allergy, keep a diary, note any reactions, and ask for a referral to a paediatric dermatologist or allergist.
The vast majority of food allergy is limited to nine food groups: milk, egg, peanut, soya, wheat, tree nuts, sesame, shellfish and kiwi. Diagnosing food allergy in children up to the age of three is based on a history of symptoms. Treatment involves avoiding the food and then gradually reintroducing it. The only exceptions are peanut and shellfish as these are lifelong allergies.
Whatever happens, don’t change your baby’s diet unless you’ve been advised to by a healthcare professional, as this may affect your baby’s growth and development.
6. Which is the best emollient for my baby?
Emollients (medical moisturisers) treat dry skin by providing a surface film of oils. This increases water in the upper layer of the skin, restoring and providing a robust skin barrier, to prevent the entry of environmental agents or triggers.
Emollients soften the skin and reduce itch. If they are used regularly to maintain skin hydration, they can reduce the frequency of eczema flares. Leave-on emollients include lotions, creams,
ointments and gels.
The emollient advised or prescribed for your baby should prevent dry skin and not cause irritation. You might need to try several products until you find the right one. Apply leave-on emollients regularly, throughout the day – for example, at every nappy change and after bathing.
Use the product liberally (for a baby you should be using 250g per week). To apply the product, dot it all over the skin, and then smooth it in, using a gentle, downward, stroking motion rather than rubbing in.
7. How often should I bathe my baby?
If your baby has eczema, a daily bath with an emollient will help soothe the eczema and reduce dry skin and itching, while cleansing the skin, removing dirt and repairing the skin barrier. Use leave-on emollients instead of soaps, baby washes or bubble bath, or alternatively use emollient wash products or bath additives. Avoid any perfumed products and keep the water tepid, as heat can aggravate eczema.
8. Should I worry about using the topical steroids prescribed by my healthcare professional?
No, you don’t need to worry, as long as you follow your healthcare professional’s specific instructions. Topical steroids are first-line treatments for babies with eczema. These creams have been used to treat eczema for more than 50 years, so there is a good understanding of how they work.
If you don’t treat the eczema promptly and adequately, skin damage is far more likely to occur through scratching into the deeper layers of skin.
9. How can I stop my baby itching?
Keeping your baby’s skin well moisturised and controlling any flares are the best ways to reduce the itch.
Try to work out any individual factors that trigger your baby’s flares and try to avoid exposing them to irritants. Scratching is a response to itch – but it can become a habit, too. So, keep your baby’s nails short and use sleepsuits with built-in mittens. Keep the bedroom cool: around 18°C.
10. What should I do if my baby’s eczema gets worse?
If your baby has wet, weepy skin (perhaps with golden crusting) and their eczema is not getting better with steroids, their skin may be infected and they may need antibiotics. If your baby’s eczema flare does not get better with the standard treatments recommended by the National Institute for Health and Care Excellence (NICE), your GP should refer them to a dermatology specialist. If they suspect an allergy, they should refer them to an allergist or joint dermatology–allergy clinic.
Help is out there
If your baby has eczema it’s understandable to feel worried, but you are not alone. If there’s anything you are unsure about, talk to your health visitor or GP.
