Facial eczema
Jump to:
Introduction
Eczema often affects the face, and facial eczema can be particularly distressing because it is so visible. In addition, facial skin is very sensitive, and even the mildest degree of inflammation can feel sore, itchy and uncomfortable. For some individuals, facial eczema is a short-lived problem, lasting only a week or two. For others, it may be more long-standing, with a negative impact on quality of life. Like eczema on other areas of the body, affected skin is red or darker than a person’s normal skin colour, depending on skin tone; dry and flaky; and sometimes weepy, crusty, or blistered. In skin of colour, areas affected by eczema can become darker as skin pigmentation is affected by inflammation, and then, as eczema resolves, the skin can become lighter. If the skin around and under the eyes is repeatedly rubbed, it can take on a temporary wrinkled appearance. In people with atopic eczema, permanent folds under the eyes can be seen. These are genetic and are known as ‘Dennie-Morgan folds’.
Facial eczema may occur in isolation or as part of a generalised eczema. Often there is no identifiable cause, especially when there is a history of atopic eczema or chronic eczema affecting other body areas. Sometimes, contact dermatitis, a type of eczema caused by contact with an external irritant or allergen, can be the cause of facial eczema. This can occur in anyone, even in people with no history of eczema, and can be caused by a variety of substances. These include facial products, airborne allergens at home and at work, and even nail products (varnish and gel nails). If allergy is suspected, a referral to a dermatologist for patch testing is often required, as it is not always possible to tell if someone has an allergic facial eczema by appearance alone.
Atopic eczema
This is the most common form of eczema in childhood. The cheeks are one of the first parts of the body to be affected by infantile eczema, and this usually occurs within the first few months of life. When a baby starts weaning, eczema is common around the mouth. After a year, eczema typically spreads to other areas, such as the arm and leg folds. Affected skin is red or darker than the child’s normal skin colour, depending on skin tone; dry, flaky and itchy; and at times may become weepy and crusty or blistered. Weeping and crusting can be a sign of a bacterial infection. In babies under one year, facial eczema is very common around the neck folds and cheeks, but eyelid involvement is rare. In older children, the whole face and eyelids can be affected, especially if the child also has hay fever. All children who have had eczema will be left with sensitive skin, and eczema can return at any age. Adults with atopic eczema often have facial involvement, which can be a persistent area of eczema, and often related to contact dermatitis.
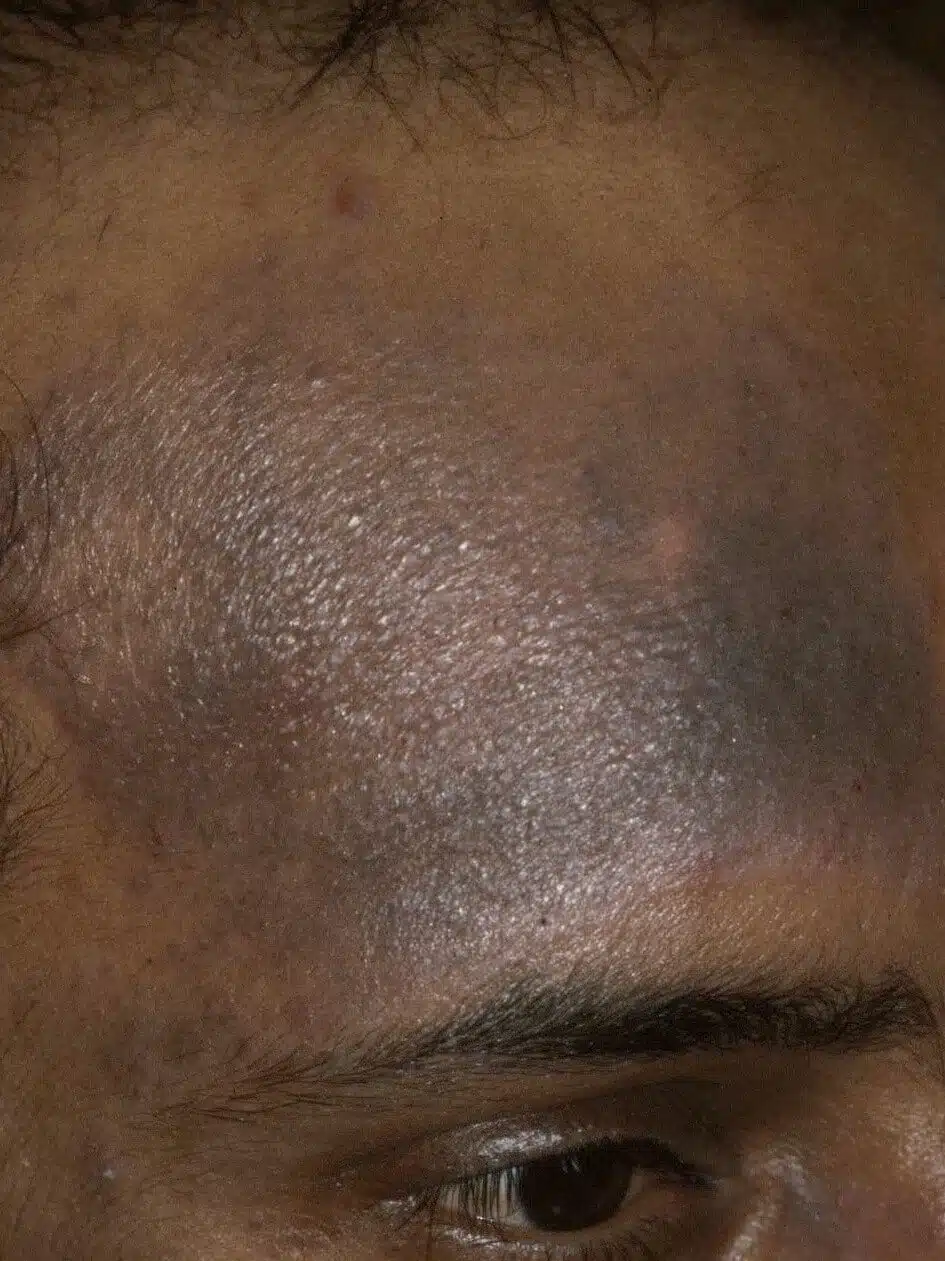
Seborrhoeic dermatitis
Probably the most common form of facial eczema in adults, this condition is often mild, appearing simply as dry, scaly skin around the creases of the ears and eyebrows. However, some people suffer from considerable irritation and soreness, especially when the eyelids or ear canals are involved.
Dandruff is an example of mild seborrhoeic dermatitis of the scalp. Like seborrhoeic dermatitis elsewhere, it tends to be a long-term complaint, which can improve with treatment, but cannot be permanently cured.
Seborrhoeic dermatitis may also occur on other parts of the body including the scalp and upper chest. Affected areas tend to be those with high levels of skin grease (sebum). This encourages overgrowth of a skin yeast called Malassezia, which appears to trigger an inflammatory reaction in people who have become sensitised to it. To reduce yeast levels, anti-yeast shampoos and creams (for example, ketoconazole) are widely used in the management of seborrhoeic dermatitis.
Environmental factors such as sun, temperature and humidity may also trigger flares, and the condition tends to worsen when an individual is run down or under prolonged psychological stress.
Babies often develop seborrhoeic dermatitis on the scalp (this is known as ‘cradle cap’). This can occur in any infant and usually resolves by 6-12 months of age. It is different from adult seborrhoeic dermatitis, as it has a different cause.
For more information, see National Eczema Society’s factsheets on Seborrhoeic dermatitis and cradle cap in infants and Seborrhoeic dermatitis in adults.
Irritant contact dermatitis
Most people use a range of cosmetics and toiletries in daily life and these can cause irritation. Examples include soap, foaming washes, exfoliating scrubs, cleansers, toners, make-up, sunscreens and shaving foam. Overuse and even limited use, especially in someone with an eczema tendency, can lead to dryness and soreness of the skin. Even products labelled ‘dermatologically-tested’, ‘natural’ or ‘organic’ can cause irritation. None of these terms guarantees that a product will be trouble-free, especially if it is used by someone with an existing facial eczema. Cosmetic products should be avoided when facial eczema is active, as they are only intended for use on normal/unaffected skin.
Changes in temperature and humidity often aggravate eczema. Some people find that their skin improves in the summer, while others find that hot weather makes them itch and scratch more. Many find that their skin tends to be worse in the winter, when the face, in particular, is exposed to harsh winds, rain, sleet and snow. Moving from the cold into the dry heat of centrally heated buildings can also make the condition worse.
Children, in particular, occasionally suffer from a localised type of irritant contact dermatitis around the lips, as a result of repeated licking, known as ‘lip-licking dermatitis’. The habit arises because the person finds that their dry lips are temporarily more comfortable after being licked, but in the long-term, the repeated contact between saliva and skin does more harm than good.
Teething, too, commonly causes irritant contact dermatitis around the mouth and chin due to the constant wetness and irritation from dribbling.
In addition, runny noses and messy foods when weaning can cause problems. Baby wipes containing irritants such as alcohol and fragrance can dry out and irritate the skin. It is best to use damp cotton pads with emollient on them as an alternative to baby wipes.
Allergic contact dermatitis
Allergic contact dermatitis occurs when the immune system in the skin overreacts to what has, until this point, been a harmless substance. The face is one of the most common sites for allergic contact dermatitis because facial skin comes into contact with many potential allergens in daily life.
The most common causes of allergic contact dermatitis on the face are fragrances/perfumes (both natural and synthetic) and preservative chemicals in toiletries and cosmetics (e.g. methylchloroisothiazolinone (MCI) and methylisothiazolinone (MI), also known as Kathon CG (MCI/MI)). Other common allergens include hair dye and nail varnish (nail varnish and gel allergy often appear on the face rather than the nail area, due to fingers touching the face). An allergy that has become more prevalent in recent years is methacrylate allergy. This has increased with the demand for acrylic nails.
In rare instances, a person can be affected by airborne, volatile allergens such as industrial chemicals or glues, which find their way onto the face and neck.
People often assume that because they have used a product such as hair dye for several years without any problems, they cannot be allergic to it. Actually, it is the other way around – the more you apply a potential allergen to your skin, the more likely it is that you will one day become allergic to it! This is called a ‘type IV delayed sensitivity reaction’.
Sometimes, people develop an allergic skin reaction to the treatments used for their facial eczema or for related/unrelated conditions on or around the face (e.g. antibiotic ear drops or eye drops). This may give the impression that a treatment is not working because the rash persists as long as the problematic cream/ointment/medication is used. It can sometimes be difficult to tell the difference by appearance alone between a skin infection and a strong allergic reaction.
Allergic contact dermatitis is worse on the area of skin that has been in direct contact with the allergen – so lipstick allergy affects the lips, mascara allergy affects the eyelids etc. Nickel allergy remains one of the most common allergies in women, who often develop it after repeatedly wearing jewellery containing inexpensive metal – this is especially the case with earrings worn in pierced ears.
Allergic contact dermatitis is an example of a delayed allergy reaction as it appears over several hours or days. It is not to be confused with an immediate stinging or itchy sensation after applying a substance, which is usually just a sign of sensitive skin. The delayed onset of an allergic reaction can make it difficult for the affected person to pinpoint what has caused the problem.
Patch testing can help identify if someone has allergic contact dermatitis. It involves the application of small quantities of allergens to skin unaffected by eczema, usually on the upper back. This area of skin must be kept dry and will be examined over several days to see if there is a reaction. Patch testing is a very safe and useful way to investigate suspected allergic contact dermatitis, but it can take considerable skill to interpret the results, and should only be carried out by a specialist who has had appropriate training. Once an allergen has been identified, it is important to avoid or minimise contact with it in the future, as there is at present no way of reversing a skin allergy.
Light sensitive eczema
Many people with eczema find that their skin improves in warm, sunny weather, and phototherapy (a prescribed course of ultraviolet therapy, administered and supervised in a hospital dermatology department) is an additional treatment option for chronic, widespread eczema. However, some people with atopic eczema or facial seborrhoeic dermatitis notice that their skin worsens in strong sunlight.
Certain medications for other conditions can cause an individual to become more sensitive to sunlight, and burn easily, and this often shows up on the face, upper neck and backs of the hands, as these are the body parts that are most frequently exposed to the light. Examples of such medications include some diuretic tablets taken for high blood pressure, and antibiotics. Shaded areas, such as under the chin and behind the ears, tend not to be affected, and this can be a helpful clue that sunlight sensitivity is a problem.
Occasionally, allergic light-sensitive eczema can be caused by touching plants followed by sun exposure (known as ‘phytophotodermatitis’).
Chronic actinic dermatitis is a rare and particularly severe form of sun sensitivity that usually affects older men, and may follow a previous allergic contact dermatitis. High factor sunscreens (SPF50) are important for treatment of this type of eczema, but it is important to find a sunscreen that suits you and does not cause further irritation or allergy. Sunscreens can be prescribed for light sensitive conditions.
Treatment of facial eczema
Eczema on the face requires careful treatment as facial skin is more easily irritated by and vulnerable to the side effects of topical therapy. It is important to consider the possibility of an allergic contact dermatitis in anyone with a persistent facial eczema, even if they have a long-standing, in-built eczema tendency.
It is helpful to make a diagnosis of which particular type of facial eczema someone has in order to know which treatment is likely to work best, and to help give an idea of the expected outcome. Usually, as eczema is a chronic condition, controlling facial eczema and preventing flares will be the main focus of treatment. In general, treatment of facial eczema involves avoiding further irritation caused by cosmetics and toiletries, switching to a gentle regimen of skin cleansing, and actively treating the eczema with emollients and anti-inflammatory therapy (topical steroids for flares and topical calcineurin inhibitors for longer-term treatment and maintenance). For more information on both treatments, please see National Eczema Society’s factsheets on Topical steroids and Topical calcineurin inhibitors.
Practical points
- To cleanse the skin and remove scaling, use a medical emollient as a soap substitute. Avoid cosmetic skin cleansers as they generally contain detergent and fragrance.
- Gently pat the skin with a soft towel to dry it – do not rub.
- Avoid soap, detergents, exfoliating scrubs and toners.
- Apply a bland medical emollient at least twice a day to sore, dry areas.
- Avoid cosmetic moisturisers as these usually contain a much larger number of ingredients and potential allergens than simple medical emollients.
- Products labelled as ‘natural’, ‘dermatologically-tested’ or ‘hypoallergenic’ can cause both irritant and allergic reactions.
- Make-up can irritate facial eczema, especially liquid foundation and mascara, so do not use it on affected areas. Mineral make-up is generally less irritant for people with eczema.
- Remove make-up with emollient on a damp cotton pad. Emollients are just as efficient and effective as cosmetic make-up remover products.
- If you suspect that your make-up may be an irritant, stop using it and re-introduce products one at a time, to see if any particular product is causing irritation.
- Apply a mild potency steroid cream or ointment to affected areas once a day, or as prescribed, for a short treatment burst (usually up to two weeks). These are best applied at night before bed. If your facial eczema is more severe you may be prescribed a moderately potent topical steroid for a short treatment burst.
- Moderate potency steroids may sometimes be prescribed for more severe facial eczema, for a short treatment burst (usually two weeks). One daily application is adequate, usually at night before bed.
- Potent steroids should never be used on the face, except under the close supervision of a dermatologist. They carry a higher risk of skin-thinning and permanent damage.
- Very potent topical steroids should never be used around the eyes.
- Topical calcineurin inhibitors (Elidel and Protopic) are helpful options for the long-term management of facial eczema as they do not carry any risk of skin-thinning. Topical calcineurin inhibitors can make the skin more light sensitive, so they should be used at night or with sun protection applied two hours after application. Topical calcineurin inhibitors are only available on prescription and should be prescribed by a specialist, including GPs with a special interest in dermatology.
- Anti-yeast ointments or creams are useful for the management of seborrhoeic dermatitis, with or without a mild topical steroid.
- A sudden, painful flare of eczema with development of clustered spots and feeling unwell, can be a sign of a widespread cold sore virus, and immediate medical attention should be sought. This is a rare but serious viral infection called eczema herpeticum.
To obtain the information on this page in a PDF format, please download our Facial eczema factsheet, below. Detailed information about Seborrhoeic dermatitis can be found in our Seborrhoeic dermatitis factsheet, below.
