Eczema SOS: Getting on top of eczema flare-ups
When an eczema flare rears its head, it can feel as if your skin becomes a battlefield. Claire Moulds puts you back in control. This article was published in Exchange 182, December 2021.
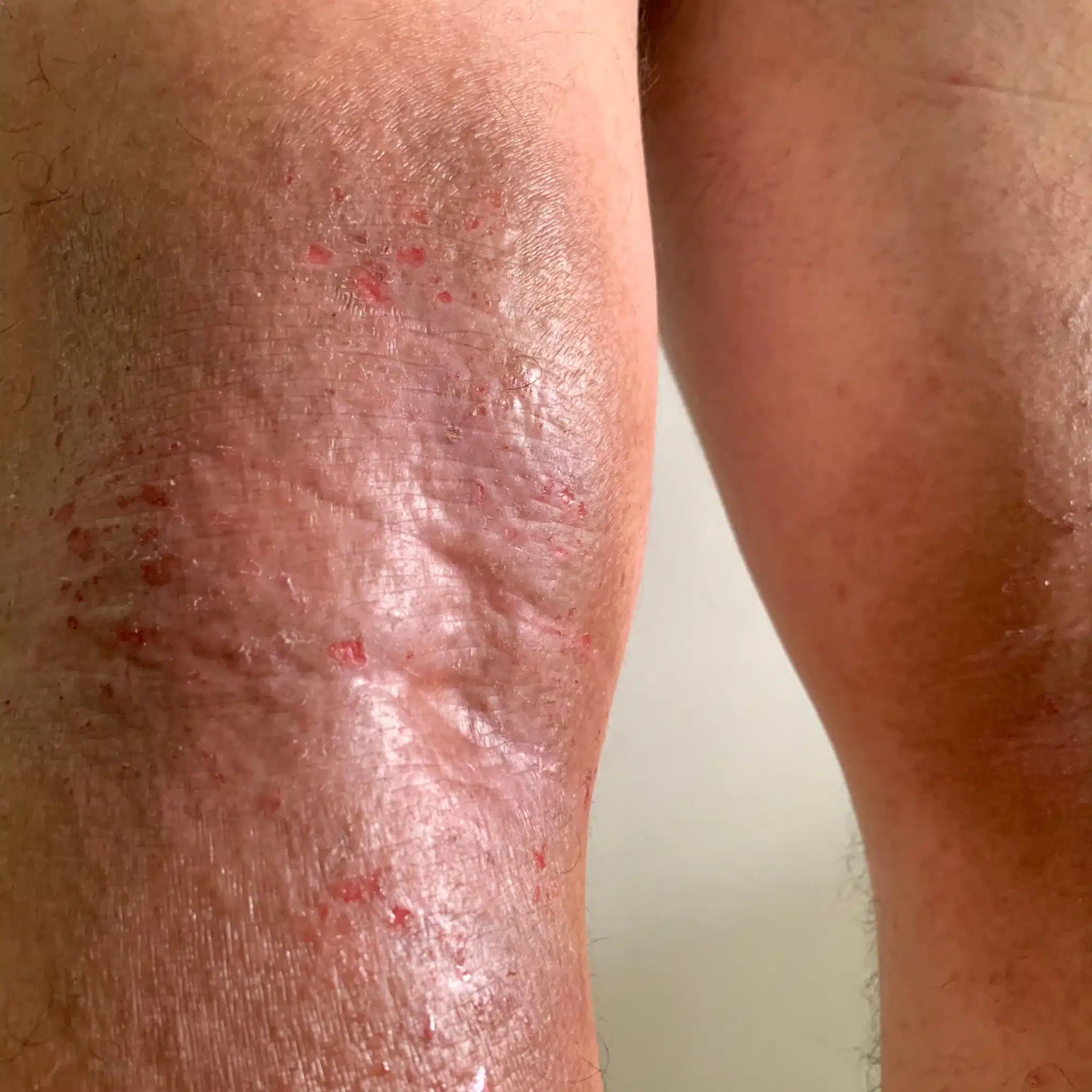
When a flare-up strikes it can feel as though you’re at the mercy of your eczema, as it becomes increasingly red (or darker than your usual skin tone, depending on skin colour), itchy and sore, due to inflammation.
Crucially, it’s vital to nip an eczema flare-up in the bud, before it can progress, to minimise its severity. Left untreated, a flare-up can easily spiral out of control, making it harder to restore your skin to its previous condition.
So, what steps can you take before, during and after a flare-up?
Preparation is key
- Make sure you fully understand how to step up your treatment regime, to treat a flare, before one occurs. This is especially true if you’re newly diagnosed. This might mean ensuring you have the relevant treatments in your bathroom cabinet, ready to be deployed, or having them on your repeat prescription, to be ordered if you feel a flare-up coming on. If your GP prefers the latter option, check that the items remain on your repeat prescription list, as sometimes these will be removed, if you haven’t used them in a while.
- Ensure you always have ample supply of your emollients and other daily medication. Running out of your ‘essentials’ is bad enough when your eczema is under control, but during a flare-up it can be a disaster!
- Be clear on how to escalate the situation if the eczema shows no improvement after a week of adhering to your flare-up plan. This process should be agreed in advance with your GP, dermatology nurse or dermatologist, so that you know how to access support quickly, and appropriate notes made on your record if required. If you’re being treated by the hospital team, but your medication is issued by your GP, it’s particularly important that everybody is on the same page.
- Arrange a chat with your employer when you first join to discuss your eczema and agree a plan when it comes to flare-ups. This might include being able to work from home on days when you’re really suffering, temporarily relocating to a different part of the building that is cooler, altering your working hours to avoid additional stress (i.e. travelling during rush hour) and how all of this will be communicated to, and managed, within the team.
- If you have caring responsibilities for young children or elderly parents, or both, put a plan in place in advance for when a flare-up means you can’t do everything that you normally do for them. Don’t wait until one strikes to try and fill the gaps! Support might come from your partner, family, friends and neighbours or temporarily from external organisations such as community groups or private agencies to ensure everyone is clean, fed and cared for.
- Check how to access emergency treatment if you go abroad and ensure you have a valid European Health Insurance Card (EHIC) or UK Global Health Insurance Card (GHIC) as well as appropriate holiday insurance. Inform the latter of your condition when taking out the policy/renewing and confirm that they will cover it.
When your skin becomes a battlefield
- During a flare-up it’s vital to rigorously adhere to your treatment plan, especially if insufficient emollient application was a contributing factor to your skin’s relapse.
- If being unwell has contributed to the current flare it’s important to treat the symptoms of that illness at the same time, rather than simply ‘soldiering on’, as your body will struggle to overcome both without help.
- A short burst of treatment with topical steroids will enable most people with eczema to bring a flare-up under control. Key points to remember include:
- The topical steroid should be used once a day – unless directed otherwise – at night for 7-14 days
- Apply with clean hands in a thin layer so that the skin glistens and wash your hands again afterwards
- Ensure you’re using the right amount as, if you don’t use enough, you aren’t properly treating the inflammation. Guidelines on the amount to cover each body area are based on the Finger Tip Unit (FTU), which is the amount of cream or ointment that just covers the end of an adult finger, from the tip to the crease of the first joint, when squeezed from an ordinary tube nozzle (see our Topical steroids factsheet for further information). If only a small part of the larger area is affected, i.e. the elbow and wrist and not the full arm, then you only need to apply topical steroid to the active areas of eczema and do not need to use the full 3FTU recommended for an entire adult arm
- If a stronger topical steroid was required to get the flare-up under control this will be ‘stepped down’, rather than simply stopping it. Topical steroids are stepped down by reducing either the frequency of application or the potency. For example, a potent topical steroid may be used once a day for seven days and then either reduced to every other day, or switched to daily use of a less potent steroid, for a further week
- If you suffer from frequent flare-ups you may be advised to apply a topical steroid on two consecutive days each week, on the areas where your eczema usually flares, as ‘maintenance therapy’ to reduce your overall number of flare-ups
- If your eczema doesn’t improve after a week, or returns soon after stopping treatment with a topical steroid, you may require a stronger steroid or additional treatment
- If the eczema gets worse and becomes sore, oozy and crusty then it may have become infected and you should seek medical advice, as it will require additional treatment.
- Keep a diary of your symptoms and a photographic record to share with healthcare professionals. Flare-ups can vary in severity, appearance and the areas affected so it’s helpful to chart how yours change over time.
- Prioritise self care as your body won’t heal if it’s run down. Get plenty of rest and sleep, eat well, drink lots of water, don’t take on too much and relax. It’s easy to say ‘I can’t’ or ‘I don’t have the time’ but, when your skin needs extra support to get back on track, you have to find a way.
- Don’t feel bad about turning down invites if you can’t face it and, equally, don’t feel compelled to attend. Make sure those closest to you know what a flare-up is like and what it takes out of you, so they understand why sometimes you’ll need to duck out of plans.
- Ensure you have a support team of family and friends around you who can help pick you up, if your flare-up is getting you down, as well as providing practical support such as food shopping.
Knowledge is power
- There may be an obvious reason for your recent flare-up, but often there isn’t. Don’t worry if you don’t know what caused it but, if you can see a pattern, make a note of what you need to avoid/do in the future.
- Learn what your skin responds well to during a flare-up, in addition to medication. An extra hour of sleep, a lighter or heavier emollient, keeping cool or getting plenty of fresh air – everyone has certain things that their skin prefers and/or which make them feel better during a flare-up. You just need to work out the right combination for you!
- If you’ve experienced a succession of bad flares and feel that your eczema is no longer under control, even outside of these, make an appointment to discuss the situation with your care team as your day-to-day treatment regime may need amending as well as your flare-up plan.
