Pompholyx eczema
Jump to:
Additional treatments for severe pompholyx
Introduction
Pompholyx eczema (also known as ‘dyshidrotic eczema’) is a type of eczema that affects the hands and feet. It involves the development of intensely itchy, watery blisters, affecting the sides of the fingers, the palms of the hands and soles of the feet. Some people have pompholyx eczema on their hands and/or feet with other types of eczema elsewhere on the body. This condition can occur at any age but is usually seen in adults under 40, and is more common in women.
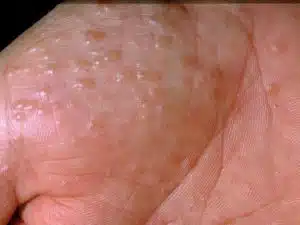
© Professor Raimo Suhonen. This image is used with the permission of DermNet New Zealand, www.dermnetnz.org
The skin is initially very itchy with a burning or prickling sensation. Then comes a sudden crop of small blisters (vesicles), which turn into bigger, weepy blisters, which can become infected. When the skin is infected, there is inflammation, irritation/pain, swelling and pustules. There is often subsequent peeling as the skin dries out, and people of any skin colour can experience skin that is red or darker than the surrounding skin and dry, with painful cracks (skin fissures). Pompholyx eczema can also affect the nail folds and skin around the nails, causing swelling (paronychia).
What causes it?
The exact causes of pompholyx eczema are not known. It is thought that stress, sensitivity to metal compounds (such as nickel, cobalt or chromate), heat and sweating can aggravate this condition. Fifty percent (50%) of people with pompholyx have atopic eczema as well, or a family history of atopic eczema. Pompholyx eczema can coexist with fungal infections, so assessment should include checking for the presence of any fungal infection on the hands and/or feet.
Pompholyx eczema occurs on the palms of the hands, fingers and feet. The skin in these areas is particularly prone to exposure to potential sources of irritation and aggravation. For this reason, pompholyx eczema can be debilitating and difficult to manage. It can also cause problems with employment.
The hands and feet are also prone to contact dermatitis. This can take one of two forms: irritant contact dermatitis or allergic contact dermatitis.
An irritant reaction could be the result of contact with potential irritants such as soap, detergents, solvents, acids/alkalis, chemicals and soil.
Or there could be an allergic reaction to a substance that is not commonly regarded as an irritant, such as rubber, nickel, or dyes in leather shoes. It is possible to have been in contact with a substance for years without any problems and then suddenly develop a sensitivity to it. If you identify a pattern, tell your GP, as patch testing may be appropriate. Patch testing is carried out in suspected cases of allergic contact dermatitis, not irritant contact dermatitis.
Pompholyx can occur as a single episode, but for most people, it is a chronic type of eczema that will come and go with a flare lasting 2-3 weeks.
Treatment
Any obvious trigger for the pompholyx flare should be avoided as far as possible, especially in the case of a contact allergy.
Emollients (medical moisturisers) are a first-line treatment and should be used for moisturising and washing.
If your skin is weeping, oozing and crusting, a potassium permanganate soak may be advised. Potassium permanganate is a chemical that can be obtained as a ‘tablet’, solution or crystals. It is for external use only, which means it should never be put in the mouth or swallowed. It is usually obtained on prescription (generally as Permitabs) but can be bought over the counter from a pharmacy. We recommend speaking to a healthcare professional before using it. Potassium permanganate soaks can be used once or twice a week.
Wearing disposable protective gloves, use a clean container (such as a large saucepan, bucket or washing-up bowl) lined with a clean white bin liner bag. A white bin liner bag will allow you to see the colour of the water when potassium permanganate is diluted with it. Fill the lined container with 4 litres of warm tap water and add one tablet – allow the tablet to dissolve completely in the water. The colour of the water should be light pink, or the colour of rosé wine. Soak the hands and/or feet in this solution for 10-15 minutes. Then rinse them in water with emollient, and pat them dry with a clean towel.
Potassium permanganate will stain the skin and the container, which is why it is advisable to wear gloves when handling it, and to use a saucepan, bucket or washing-up bowl lined with a bin liner bag as the container. It is also a good idea to apply petroleum jelly (for example, Vaseline) to the nails beforehand to prevent staining. After using the soaks, continue to moisturise your hands and/or feet with emollient.
When the acute flare of pompholyx subsides, the soaks should be stopped (usually after 3-7 days).
A leave-on emollient or an emollient soap substitute should be used for washing, since soap de-greases the skin and can also act as an irritant. During the Covid-19 pandemic, people with eczema were advised to wash their hands first with soap and then with an emollient, as emollients were not considered effective at removing Covid-19 particles. It is a good idea to carry around a small dispenser or pot of emollient to use for hand-washing during the day. For more information and practical tips on emollients, please see National Eczema Society’s Emollients factsheet.
Pompholyx eczema needs to be treated with topical steroids to reduce inflammation and heal cracks. Hands usually require stronger steroids (the skin of the palms is thick), so potent topical steroids are usually prescribed for adults (moderately potent for children). They should be used for a short treatment burst – generally 2 weeks. For more information, see National Eczema Society’s factsheet on Topical steroids. Topical steroids will need to be prescribed by your GP or other healthcare professional. Topical steroids switch off the inflammatory response, but as they reduce the inflammatory process, the skin can become drier, so you will need to apply emollient frequently.
If your hands and/or feet are sore and weepy, and yellow crusting is present, you may have a bacterial infection. This will require a course of oral antibiotics, prescribed by a healthcare professional.
Additional treatments for severe pompholyx
For severe pompholyx eczema, a dermatology referral may be required for treatment and/or diagnosing contact allergy through patch testing. Treatment may include a short course of an immunosuppressant drug. Alitretinoin (known as Toctino) is an oral treatment licensed for use in adults with severe chronic hand eczema (including pompholyx) that has not responded to treatment with potent topical steroids. Alitretinoin works by reducing the inflammation associated with eczema as well as damping down the response of the immune system. It is a capsule that is taken by mouth once a day with a meal for 12-24 weeks, depending on how the condition responds to the treatment.
Alitretinoin can only be prescribed by dermatologists or doctors with experience both in managing severe hand eczema and in the use of retinoids. The specialist will determine whether your hand eczema is severe by examining your hands and asking a series of questions about how the eczema affects your life. You will need to be carefully monitored.
Retinoids are likely to cause severe birth defects if taken during pregnancy. This means that anyone with childbearing potential must avoid becoming pregnant during treatment and for one month after stopping treatment – for example, by using two effective methods of contraception. The drug can only be prescribed if a pregnancy test is negative. Regular pregnancy tests will be taken during treatment.
You should not breastfeed while taking alitretinoin and for a month after completing treatment.
The most common side effects are headaches, dry lips and skin, and flushing. Other side effects include raised blood fats such as cholesterol, and decreased levels of thyroid hormone. Due to potential side effects, a lower dose will be prescribed if you are diabetic.
Phototherapy (UVB or PUVA), using either UVB or UVA rays administered by a special foot/hand light box, may be recommended if this treatment option is available locally to you. Assessment and treatment (2-3 times a week) usually takes place in a dermatology department. In some areas of the UK, you may be loaned a light box so you can administer your treatment at home, although you will continue to be monitored by the dermatology department. Phototherapy treatment is usually carried out for 12-16 weeks.
Occasionally, for very severe outbreaks of pompholyx eczema, a short course of oral steroid tablets is prescribed.
Practical management
- Use lukewarm water for washing as very hot or cold water may irritate the skin. Remember to use an emollient as a soap substitute.
- Try to avoid direct contact with detergents and cleansing agents. Wear 100% cotton gloves under rubber or plastic gloves when carrying out household tasks. When shampooing your hair, wear cotton gloves under waterproof gloves, as above. If possible, when the pompholyx is active, ask someone else to do the shampooing for you – and the housework, too!
- If itchiness is interfering with sleep, sedating antihistamines may be helpful at night (but will cause unwelcome drowsiness if taken during the day). Remember, antihistamines in eczema aid sleep rather than actively treat itch.
- Large blisters may be gently drained by using a large sterile needle. Very gently make a small jagged tear in the blister (a pin-prick hole will not be effective as it will not release fluid and will seal up very quickly). Make sure you do not remove the ‘roof’ of the blister – this protective layer of skin needs to stay in place, otherwise soreness can increase, healing can be delayed and there is a risk of infection.
- Socks, tights and gloves should be made from cotton, bamboo or silk (as close to 100% of these different materials as possible), as synthetic materials such as nylon are less absorbent and do not generally allow the skin to ‘breathe’ in the same way.
- Bandaging or wrapping the hands and/or feet can help protect the skin. Alternatively, cotton, bamboo or silk gloves or socks can be worn. Covering the skin can bring some relief as well as ensuring that creams and ointments are given the maximum opportunity for absorption. If paste bandages or wet wraps are used, you should consult a healthcare professional about their suitability, how to put them on, and how to use them with creams and ointments. Any weeping blisters should be covered with a non-stick dressing, to prevent tearing the blister roof.
- For severe cracks, a steroid impregnated tape can be applied to protect them and speed up healing. It would need to be prescribed by a healthcare professional.
- If you have painful cracks post-blister stage, Extra Thin Duoderm is a helpful hydrocolloid dressing that you can cut to shape and put on cracks. It can be left in place undisturbed for a few days. Speak to a healthcare professional before using Duoderm on an area you are treating with topical steroids, because when you closely cover skin that is being treated by a topical steroid, this will make the topical steroid more potent.
- Footwear should be kept dry and permeable to the air. Avoid plastic or rubber shoes, or any other type of footwear likely to cause sweating. Light shoes with cotton linings are preferable to shoes with synthetic linings.
To obtain the information on this page in a PDF format, please download our Pompholyx eczema factsheet, below.
