Discoid eczema
Jump to:
What does discoid eczema look like?
Can discoid eczema become infected?
How is discoid eczema treated?
Introduction
Discoid eczema is a fairly common type of eczema, seen in people with and without a history of
atopic eczema. It has a distinctive appearance with oval or round lesions, and can be very itchy.
There are a number of things you can do at home to improve discoid eczema, as well as a variety of
treatments you can get on prescription from your healthcare professional.
Who gets discoid eczema?
Discoid eczema (also known as nummular eczema/dermatitis) can occur at any age, including childhood, but is seen more frequently in adults. Anyone can develop discoid eczema, but people with atopic eczema, people who had eczema as a child, people with infected eczema and people with allergic contact dermatitis are more likely to develop it. There is also an association with chronic alcoholism, which is confirmed by abnormal liver function blood tests.
What causes discoid eczema?
The exact cause of discoid eczema is not known, although dry skin is perhaps the most common feature. People who had atopic eczema in childhood are often left with dry skin – these people may develop discoid eczema as adults, particularly on the hands. Others with no history of eczema but who nevertheless have ‘sensitive skin’, which is drier than normal, can also develop discoid eczema, often in middle age or later.
Children and adults with atopic eczema can present with discoid eczema or a mixture of both flexural eczema (eczema in the skin creases) and discoid eczema. Children of colour are more likely to develop discoid eczema than white children.
Discoid eczema is more common in the cold winter months, when our skin is exposed to central heating, dry air (low humidity) and fan heaters, which all dry the skin. Frequent contact with degreasing agents can remove the natural oils of the skin, leaving it dry and cracked, and causing an irritant contact dermatitis. Older people, whose skin is drier and thinner, can be more prone to discoid eczema especially if they have varicose and asteatotic eczema.
Discoid eczema can also develop on an area of skin that has been damaged or scarred from a scratch, bite, burn or localised area of infection. It can sometimes be triggered by drugs, especially medications that have a side effect of skin dryness.
When discs are seen in an unusual place, this might be a contact allergy rather than discoid eczema. For example, jean studs or belt buckles can cause a rash that looks like discoid eczema but is, in fact, due to an allergy to nickel. Allergic contact dermatitis is often one patch, whereas discoid eczema tends to present as several patches scattered around the body. If allergic contact dermatitis is suspected, you may be referred to a dermatologist for patch testing, to help find out the cause of the allergy.
Stress may play a part in the development of discoid eczema, but is unlikely to be the sole cause of it. Worry can make the condition worse, or more long-lasting. Any sources of concern should be addressed, if possible.
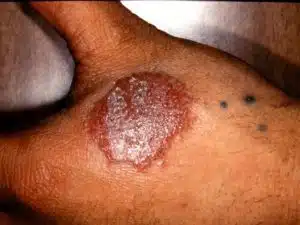
What does discoid eczema look like?
This image is used with the permission of DermNet New Zealand, www.dermnetnz.org
Another name for discoid eczema is ‘nummular’ eczema,
which means ‘coin-shaped’ eczema. It usually appears
quite suddenly on the first occasion, when one or two
round or oval patches appear. These are a dull red colour
or a darker shade than your usual skin colour, depending
on skin tone, and the size of a 50 pence piece or smaller. These patches start off with a slightly bumpy surface and fuzzy edges, usually on the lower legs, trunk or forearms, although hands and fingers can also be affected. Within a few days the patches often develop raised lumps or blisters which start to ooze, and they can become very itchy, crusted and infected. Later on, the surface becomes scaly and the centres of the discs clear, leaving the skin dry and flaky. At any time between 10 days and a few months later, other discs may appear, often in the same position on the opposite side of the body – other patches may then come up in different places, such as on limbs previously not affected. Old patches that have apparently cleared up may also reappear.
This image is used with the permission of DermNet New Zealand, www.dermnetnz.org
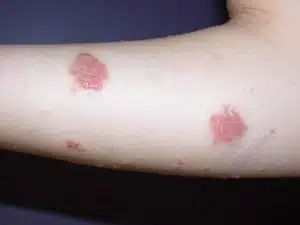
With treatment, the condition can improve, although
discoid eczema does tend to recur and may leave pale
areas (post-inflammatory hypo-pigmentation) and dark
areas (hyper-pigmentation) in people with darker skin
tones. Usually, the skin returns to a perfectly normal
appearance after several months, and scarring is very
rare. Discoid eczema can remit and relapse and is more
likely to return in the colder winter months. Discoid
eczema can also resolve completely for some people.
Can discoid eczema become infected?
Yes – when patches of affected skin begin to weep and itch, the chances of that site becoming infected with bacteria are high, particularly if scratched. Sometimes a skin infection may spark off a flare of discoid eczema. If the surface has a yellow crust or is very weepy, the skin is probably infected and you should see a healthcare professional to get treatment. The condition can become more widespread if any infection is left untreated, while treatment of the infection can help clear up the eczema.
How is discoid eczema treated?
A number of medications are available from your GP to help treat discoid eczema, and there are steps you can take at home to make the skin more comfortable. See your GP for a diagnosis (and treatment) if you think you may have discoid eczema. Other skin conditions, such as ringworm (fungal infections) and psoriasis can look similar.
That said, fungal infections tend to be solitary patches, and are not generally very itchy. It is unusual for fungal infections to manifest as scattered patches over the body, like discoid eczema. Psoriasis is another common skin condition and appears on the body as scaly plaques (again, round or oval-shaped areas). Psoriasis is generally not as itchy as eczema, and appears in a symmetrical pattern, commonly on the fronts of the knees and elbows. There is often scalp involvement in psoriasis. There are also some very rare skin conditions that may look like discoid eczema, so always confirm the diagnosis with your healthcare professional.
Emollients
People with discoid eczema often have dry skin that should be treated to improve the existing eczema and help prevent further flares. A wide range of emollients, also known as moisturisers, is available to treat dry skin. Various brands can be bought from a supermarket or pharmacy, and some can be prescribed by your doctor or nurse. It is best to experiment to see which one suits you best. Emollients can and should be used for both moisturising and washing.
If areas of skin are weeping or ‘wet’ (remember this may indicate infection), a cream emollient (as opposed to an ointment emollient) is more suitable. Emollients with antimicrobial properties can also be considered.
Emollients are very safe and can be applied as often as required throughout the day and before bedtime to prevent your skin from feeling dry and becoming flaky.
It is possible to become sensitive to a particular ingredient in an emollient. See National Eczema Society’s factsheet on Emollients for more information.
Baths and showers
Bathing can make discoid eczema more comfortable by removing crusts and reducing itchiness, but hot water can aggravate the condition, so baths should be lukewarm. An emollient should always be used as a soap substitute when bathing and showering. Emollient bath oils can also be used in the bath, but they are not generally prescribed. Apply more leave-on emollient after bathing and showering.
Topical steroids
Once discoid eczema has developed, the skin can become itchy and red or darker than your usual skin colour, depending on skin tone. If this happens, your doctor may prescribe a steroid with a cream or ointment base to apply to the affected areas to help them clear up. The potency (strength) of the steroid used will depend on the severity of the eczema. Generally, for adults with discoid eczema, a more potent steroid will be used for longer periods, e.g. 2-4 weeks depending on the area of the body. Children with discoid eczema will be prescribed topical steroids according to their age and eczema severity (these may be moderate or potent). Only use steroid creams or ointments on areas of skin with eczema, unless otherwise advised by your healthcare professional. Dry skin not affected by eczema is best treated with an emollient.
Treatments for infection
If your skin is infected (crusting, oozing and very inflamed), see your healthcare professional to get a specific treatment for this. If only a few patches are infected, a cream or ointment containing a combination of antibiotic and steroid may be prescribed. These are prescribed for a 14-day treatment course. Using them for longer may result in a resistance to the antibiotic. Other interventions that can be used include emollients with antimicrobial properties.
If the infection is more widespread, a skin swab may be taken and you will be given a course of antibiotic tablets, capsules or syrup (for children). Complete the prescribed course, even if the infection clears up before all the tablets are taken.
Environmental triggers
Contact with detergents can make you more likely to develop discoid eczema, so it is a good idea to avoid direct contact with any household cleaning agents, or wear waterproof gloves to protect your hands.
Dry air in centrally heated homes can aggravate the condition. If you place a bowl of water near each radiator, your skin is less likely to become dry. In cold weather, apply a moisturiser to your skin before going out and also at regular intervals when indoors, especially if central heating makes your home dry.
Conclusion
Discoid eczema can usually be controlled with emollients and topical steroids, and by avoiding triggers such as soaps, bubble baths and overheating. Regular use of emollients will maintain the skin barrier and prevent dryness. For severe and extensive discoid eczema, other treatments may be required, such as paste bandages, immunosuppressant drugs and light therapy. To access these treatments, you would need a referral to a dermatologist.
To obtain the information on this page in a PDF format, please download our Discoid eczema factsheet, below.
