Skin pigmentation and eczema
Jump to:
How different skin types are affected
Other skin conditions that cause pigmentary changes
References and further information
Julie Van Onselen, Dermatology Nurse Adviser to the NES, explains how issues with changes in skin pigmentation arise when normal skin colour is disrupted due to eczema. These pigmentary skin issues are more noticeable in darker skin but occur in skin of all colours. This article was published in Exchange 178, December 2020.
Which skin type are you?
Skin type is described by the Fitzpatrick classification (1), which determines the colour of skin by phototype, which depends on the amount of melanin pigment in the skin.
In this article we describe skin as ‘lighter’ or ‘darker’.
Skin types: Fitzpatrick classification, adapted from: https://dermnetnz.org/topics/skin-phototype/
| Skin type | Characteristics |
| I | White skin, freckles |
| II | Pale skin, freckles rare |
| III | Light/light brown skin, no freckles |
| IV | Light brown/olive skin, no freckles |
| V | Skin brown |
| VI | Skin black |
Skin changes are caused either by active eczema or by scratching as a result of eczema itch. These changes can result in two types of pigmentary skin changes in eczema:
- HYPO-PIGMENTATION Loss of skin pigment or colour, usually seen as patches of skin that are lighter than overall skin tone.
- HYPER-PIGMENTATION Patches of skin becoming darker than the normal skin tone.
Hypo- and hyper-pigmentation are more visible in darker skin types but can occur in any skin type and can be concerning and distressing for anyone with eczema.
The main way of improving skin pigmentation changes is to treat the underlying eczema and inflammation. But discoloration can last for months or years, even after the eczema is treated.
How different skin types are affected
The features of eczema differ depending on the person’s skin type.
On paler skin, the typical pattern is inflamed, red or dark pink patches, with dry itchy skin, which in severe flares may ooze with small vesicles (blisters).
On darker skin, inflammation is more difficult to detect, as it is seen as various stages of hyper-pigmentation and is more subtle, so often redness is not seen. As a result, the severity of eczema can be underestimated.
Post-inflammatory hypo- and hyper-pigmentation are a much greater concern in people with darker skin, as it can take months for this to resolve and the discoloration can sometimes be a greater concern than the eczema itself.
Another feature of eczema, more commonly found in darker skin, is follicular prominence. This is where the eczema appears in small, itchy bumps or ‘papules’ on the skin – mainly on the trunk and forearms. Dry skin and scale can also be more prominent, as its white or grey colour shows up most noticeably.
A UK longitudinal study into ethnic variations in atopic eczema reported that children with darker skin (African-Caribbean ethnicity) were more likely to develop atopic eczema than their white counterparts and were six times more likely to develop severe eczema. (2)
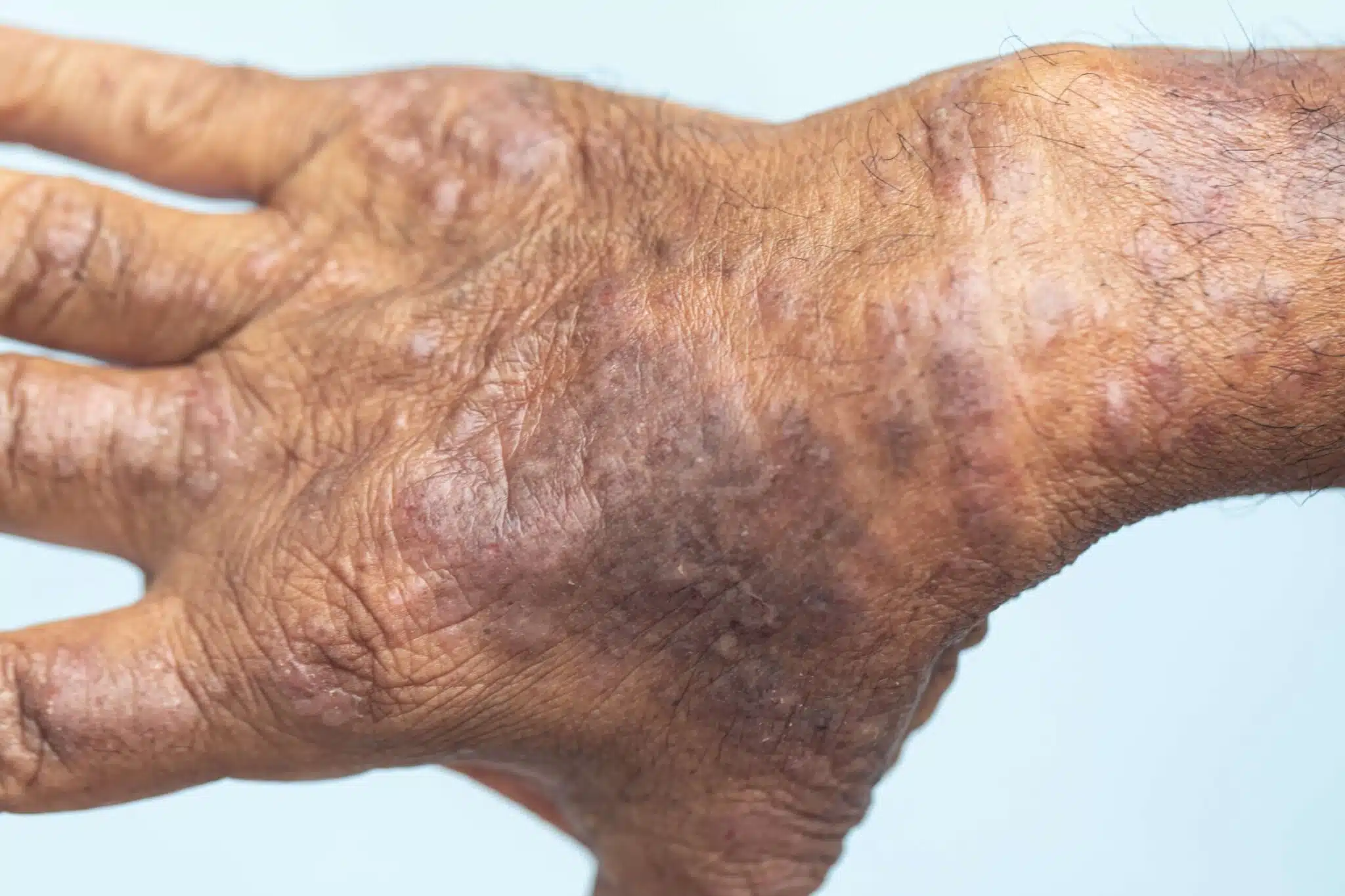
Darker patches
Darker patches of skin in eczema (hyper-pigmentation) is caused by inflammation, which stimulates the melanocytes – the skin cells that give skin its colour – to increase melanin synthesis (the process of making skin pigment). This increase in synthesis results in pigment being transferred to the skin epidermis (the top layer of the skin).
If the skin is injured by scratching or rubbing the melanin, pigment is released. This explains why people with darker skin types have hyper-pigmented areas during an eczema flare.
Post-inflammatory pigmentation
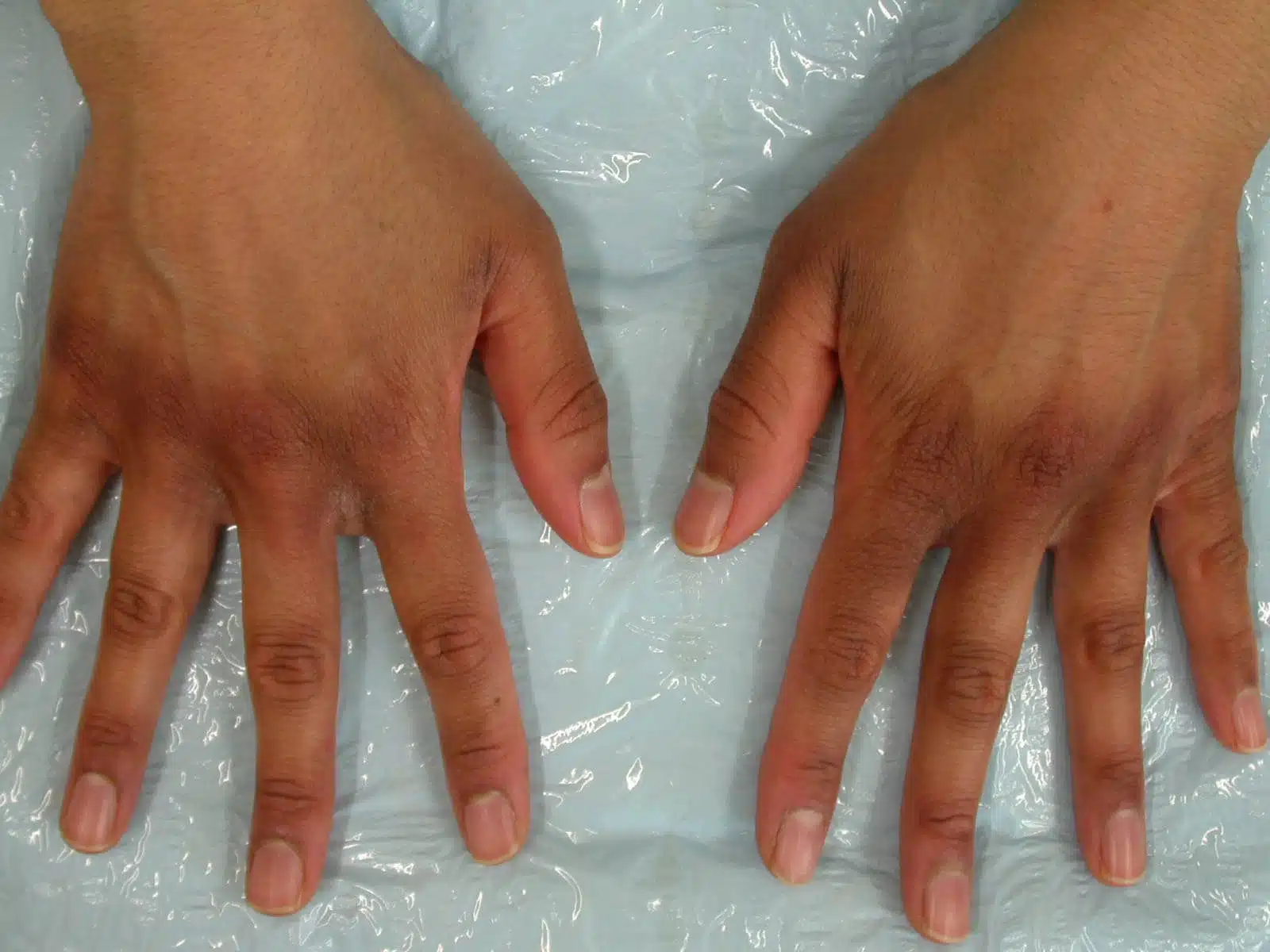
Another cause of darkening is post-inflammatory pigmentation, which can happen after the eczema flare has settled and is seen as a darker patch where eczema lesions have healed. This skin change is frustrating, as the darker patch can linger for months, even if the eczema does not return to the body site. It occurs in all skin types, but again is more apparent in darker skin. A common pigmentary feature of severe atopic eczema in all skin types is wrinkling under the eyes, known as Dennie-Morgan folds, accompanied by dark circles.
Post-inflammatory pigmentation is stimulated by sunlight, so sun protection is important for people of all skin types as it can prevent it from happening and will help it recover. Gradually, the post-inflammatory pigmentation will fade.
Lichenification
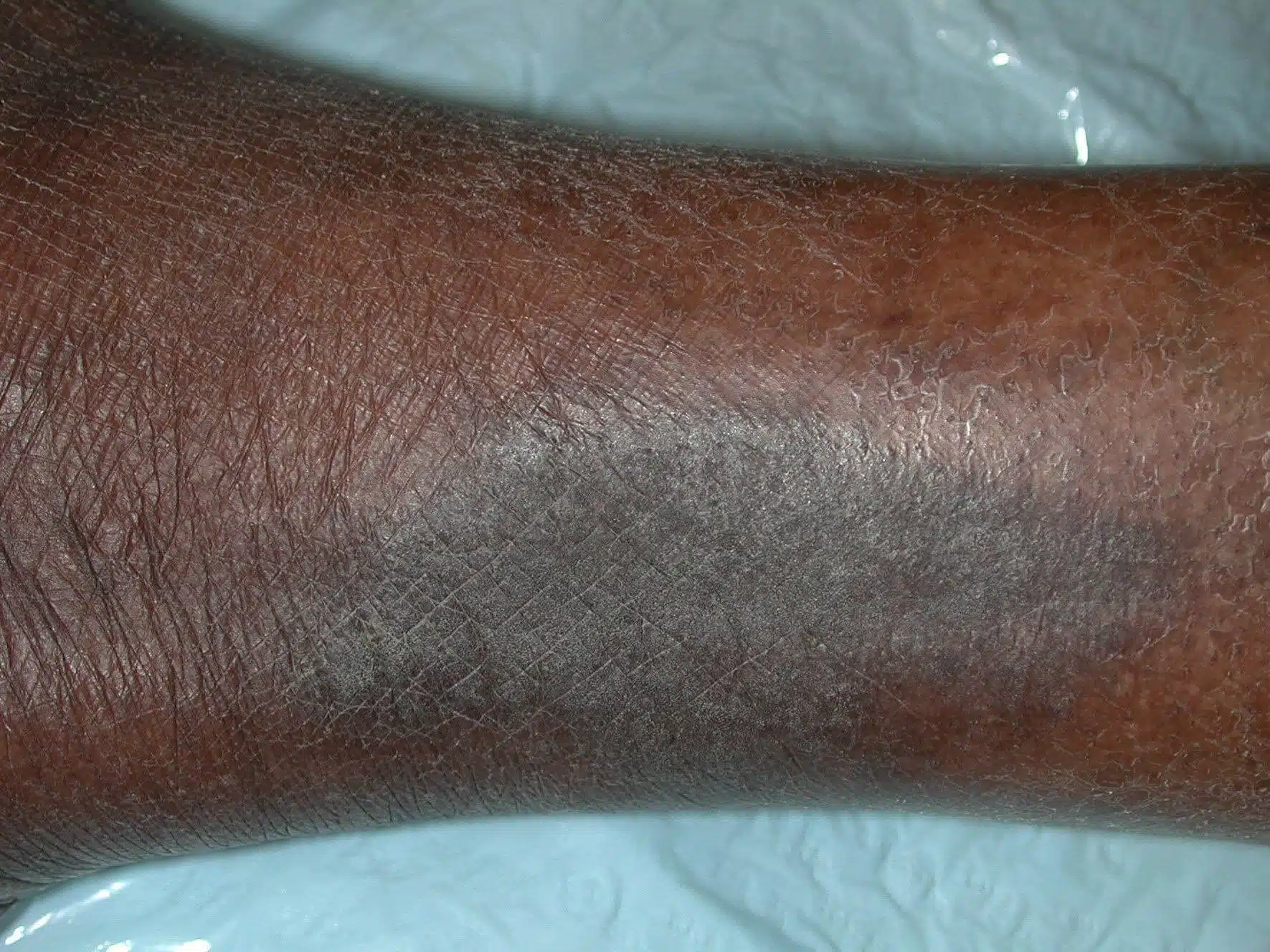
Chronic scratching and rubbing can result in thickened areas of skin with visible scratch marks and increased skin markings, called lichenification. These areas of skin are always hyper-pigmented – in pale skin it may be dark pink, while in darker skin it may be slate grey – but always dry, scaly and leathery in appearance.
Lichenification caused by constant rubbing happens in all skin types – sometimes as a single patch, usually on the person’s dominant side, such as the elbow crease on the right arm or in a specific body area. However, someone may develop a lichenified area of skin on the front of their feet simply because of a night-time habit of rubbing their feet together while they sleep.
The scratching and rubbing is often unconscious and can becomes a habit, even when eczema is not flaring. Other parts of the body where lichenification is particularly common include the back of the scalp or neck, the wrists and forearms, the lower legs and the genitals (such as the scrotum or vulva).
Lighter patches
Paler patches of skin (hypo-pigmentation) are seen when an eczema flare is resolving through the sub-acute phase and settles back to dry skin without inflammation.
People with eczema often worry that their hypo-pigmentation is caused by side-effects of a topical treatment – particularly, topical steroids. It is true that topical steroids can cause the tiny blood vessels on the skin to dilate. But this is temporary and not skin damage. The hypo-pigmentation itself is caused by the eczema, not the treatment.
Pityriasis alba
Another cause of paler patches is pityriasis alba – a low-grade eczema, mainly seen in children or teenagers. The name means ‘fine scale’ (pityriasis) and pale colour (alba) – so the patches of eczema are hypo-pigmented, sometimes pink and dry.
Pityriasis alba is more common in darker skin than white skin. It often appears following sun exposure, as the hypo-pigmented areas do not tan, making it more prominent.
The features and progression of pityriasis alba are slightly different to atopic eczema. It usually comprises between one and 20 round or oval patches, mainly on the face but also on the neck, shoulders and upper arms. Other parts of the body are unlikely to be affected. Associated dryness and scale is more apparent in the winter months, but the actual hypo-pigmentation is most apparent in the summer months.
The key difference between pityriasis alba and eczema is that it is accompanied by little or no itch. However, the two conditions often appear together, in which case the common eczema patches will be itchy. Pityriasis alba patches resolve gradually. First, the scale disappears, then the normal skin tone is restored. Again, it can sometimes take months for the skin to return to its original colour.
Treating pigmentary changes
There is no specific treatment of pigmentary skin changes but it is important that eczema is recognised and treated in people of all skin types. Prompt treatment will help minimise long-term post-inflammatory pigmentation.
Over time, hyper- and hypo-pigmentation will eventually resolve. However, it is important to remember that pigmentary changes can persist after the eczema has been successfully treated. If this happens, topical steroids should not be continued in these areas long term, as this could result in permanent hypo-pigmentation.
Other skin conditions that cause pigmentary changes
Eczema is not the only condition that causes pigmentary changes: they can also be caused by various other skin conditions that someone may have alongside their eczema. Two other common pigmentary skin conditions are melasma and vitiligo, but there are many rarer conditions too. So, any form of pigmentary skin problems that cannot be explained by eczema should be assessed and investigated.
Melasma
Hyper-pigmentation on the face – and, occasionally, the forearms – can be due to melasma, which is caused by over-production of melanin, resulting in flat, dark patches or areas of skin – most commonly on the cheeks and around the eyes. The exact cause is unknown but it can be genetic and is thought to be hormonal, as it is seen in women who are pregnant or taking oral contraceptives. It affects adults only – usually women – and is worsened by exposure to sunlight.
Vitiligo
This condition causes loss of skin colour in patches – usually permanently. The discoloured areas usually expand with time. The condition can affect the skin on any part of the body. It can also affect hair and the inside of the mouth. Treatment is aimed at restoring skin colour, but it does not prevent continued loss of skin colour or recurrence.
References and further information
References:
- Fitzpatrick TB. The validity and practicality of sun-reactive skin types I through VI. Arch Dermatol. 1988 Jun;124(6):869-71.
- Ben-Gashir B, Hay R. Reliance on erythema scores may mask severe atopic dermatitis in black children compared with their white counterparts. British Journal of Dermatology 2002;147:920-925.
Further information:
Skin Deep is a website that contains images of people with different skin tones to help patients and doctors better understand and describe symptoms of different skin conditions.
The PDF document below shows what eczema can look like on different skin tones.
